KEY ACTIVITY #19:
Provide Care Management
This key activity involves the following elements of person-centered population-based care: operationalize clinical guidelines; proactive patient outreach and engagement; care coordination; behavioral health integration; address social needs.
Overview
What is care management? How does it differ from care coordination?
Led by a care manager (a licensed clinician or a nonlicensed trained individual), care management is an intervention intended to support the highest-need individuals within your practice. The services are more targeted, require the development of a person-centered care plan, and are of higher intensity than care coordination services. A patient must consent to participate in care management activities. A care manager works directly with the patient and multidisciplinary care team members to identify, plan and implement person-centered goals and care. The care manager supports the individual in identifying and coordinating resources and referrals as well as supporting self-management activities to attain optimal wellness.
Care management provides a higher level of support to individuals who have medical, behavioral health, and/or social needs that impact their ability to access appropriate levels of care. Individuals may be receiving frequent emergency room (ER) and hospital care that could be avoided with care management activities and/or patients may have significant social barriers (housing, food and substance use) that prevent them from accessing preventative and wellness care.
Research points to care management as a potential intervention to improve outcomes for higher risk obstetric patients, such as patients at risk for preterm delivery.[1] There is a paucity of resources, however, on care management guidelines specific to the pregnant or postpartum population. Resources developed for the primary care population may need to be adjusted for the pregnant population.
Care management holistically addresses a patient’s medical, behavioral health and social health needs. Addressing health-related social needs helps in reducing health disparities among different populations. Individuals with lower socioeconomic status or limited access to resources can be provided with resources to support these areas. As part of care management, the patient’s social needs are directly addressed as part of the assessment and prioritized according to the patient's goals. For example, attaining stable housing may be the first step to achieving better health in their pregnancy.
Individuals eligible for care management have high levels of need in one or more of the domains of medical, social or behavioral health. Some examples of populations who may be eligible for care management include:
- Individuals with complex medical needs, also known as complex care management.
- Example: A patient with chronic hypertension and type 2 diabetes, currently pregnant with her fourth child.
- Goal of care management: Support optimal nutrition and medication management to minimize risks to pregnancy. Address social needs that may impact the pregnant person’s ability to manage their conditions, such as housing stability and food insecurity. Coordinate appointments for specialty visits with maternal fetal medicine.
- Individuals who require intensive support post hospital discharge / care transitions.
- Example: A postpartum patient who had severe preeclampsia and was hospitalized for four weeks at the end of her pregnancy. She has been discharged home, but her baby is still in the neonatal intensive care unit (NICU), and she is experiencing postpartum depression symptoms.
- Goal of care management: to coordinate counseling, medications, medical equipment (e.g., home BP cuff, hospital-grade lactation pump), follow up postpartum care to support optimal recovery and mental health, and minimize risk of rehospitalization.
CalAIM: Enhanced Care Management and Community Supports.
In California, Medi-Cal beneficiaries who experience high care management needs, may be eligible for a Medi-Cal benefit known as Enhanced Care Management or ECM. Beginning in 2024, this benefit will be available for pregnant and postpartum patients. ECM can be provided to eligible Medi-Cal beneficiaries at risk of poor outcomes due to high levels of medical, social and behavioral health needs. ECM delivers person-centered, trauma-informed care management services, and members can access additional services known as Community Supports to help achieve their medical and social health goals.
DHCS Enhanced Care Management (ECM) and Community Supports[2] are foundational parts of the transformation of Medi-Cal focused on:
- Breaking down the traditional walls of healthcare, extending beyond hospitals and healthcare settings into communities;
- Introducing a better way to coordinate care; and
- Providing high-need members with in-person care management where they live.
If your practice has many patients who are eligible for ECM based on descriptions below, you can contact your Medi-Cal managed care plan (MCP). Your MCP can provide you with details on patient eligibility and the requirements needed to provide ECM services to your patients. Some clinics also provide Community Supports services depending on their patient population.
ECM is available to specific groups of Medi-Cal members (called ECM populations of focus).[3]
- Adults, unaccompanied youth and children, and families experiencing homelessness.
- Adults, youth, and children who are at risk for avoidable hospital or emergency department care.
- Adults, youth, and children with serious mental health and/or substance use disorder needs.
- Adults living in the community and at risk for long-term care institutionalization.
- Adult nursing facility residents transitioning to the community.
- Children and youth enrolled in California Children’s Services (CCS) or CCS Whole Child Model with additional needs beyond their CCS condition(s).
- Children and youth involved in child welfare (foster care).
- Adults and youth who are transitioning from incarceration.
- Pregnant and postpartum individuals; birth equity population of focus (starting in 2024).
Medi-Cal members can also be connected to Community Supports services to help address their health-related social needs, such as access to healthy foods or safe housing to help with recovery from an illness. If your clinic wants to provide Community Supports services, contact your Medi-Cal managed care plan for information. Available Community Supports services include:
- Housing transition navigation services.
- Housing deposits.
- Housing tenancy and sustaining services.
- Short-term post-hospitalization housing.
- Recuperative care (medical respite).
- Day habilitation programs.
- Caregiver respite services.
- Personal care and homemaker services.
- Nursing facility transition or diversion to assisted living facilities.
- Community transition services or nursing facility transition to a home.
- Environmental accessibility adaptations (home modifications).
- Medically tailored meals and medically supportive food.
- Sobering centers.
- Asthma remediation.
How does an eligible individual get connected to ECM and Community Supports services?
The Medi-Cal managed care health plans are responsible for identifying their patients who are candidates for Enhanced Care Management and meet eligibility requirements. In addition, practices, providers and community-based organizations have the ability to refer patients for ECM services. Community-based organizations, such as homeless services providers, are a particularly valuable source of referrals into ECM, as they often have trusted relationships with individuals who may not have sought or received medical care and are therefore not known to the MCP because they have had little or no utilization of healthcare services.
How do we refer a patient who we think would benefit from ECM?
If you have a patient who may be a candidate for ECM or Community Supports services, you should contact the Medi-Cal managed care plan to inquire about services available through the patient’s health plan. Patients and family members can self-refer to ECM.
Action steps and roles
How can we provide care management services, including ECM services, in our practice?
Community practices are often well situated to provide care management services as they are the site where patients seek or can be connected to care. Clinics may decide that they want to provide care management services, including ECM services. The following resources can help assess your capacity to provide care management services within your clinic structure.
Care management for complex populations
A resource on starting a care management program for individuals with multiple medical, behavioral health and social needs is available from the Camden Coalition. This resource addresses the following areas:
- Program design: Tools to support the understanding and identification of a complex care population, plan a care model and workflow, and anticipate legal/business needs.
- Program operations: Tools to support the implementation of a complex care model including triage, outreach, engagement, intake and clinical support.
- Data and process improvement: Tools to support metric identification, data collection and analysis, and process improvement.
- Team and leadership development: Tools to support the recruitment, training and management of a complex care team.
- Community mapping and collaboration: Tools to support multisector and community coordination.
- Communication and growth of success: Tools to support broad communication and program scaling.
Care transitions
This Care Transitions Toolkit from the Indiana Patient Safety Center focuses on processes to support care management for individuals transitioning between healthcare settings.
ECM services
Aurerra Health Group’s Enhanced Care Management Provider Toolkit provides a detailed description of the services that are required to become an ECM provider. In this guide, the requirements of ECM providers are outlined in detail.
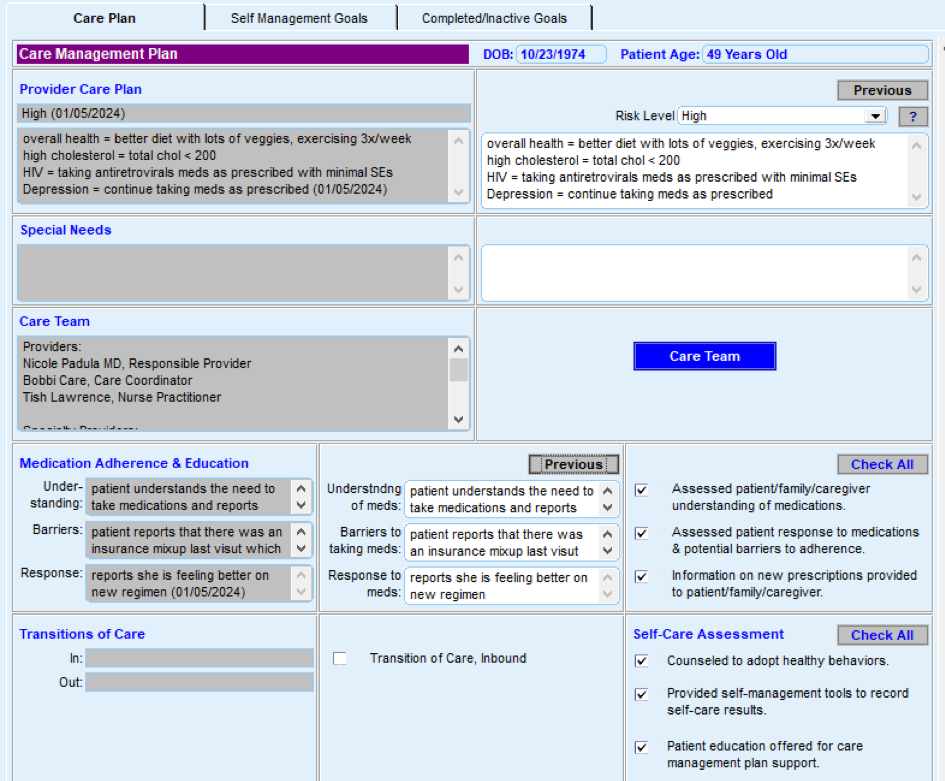
FIGURE 20: EXAMPLE OF HOW AN EHR CAN ASSIST WITH CARE MANAGEMENT
Resources
Evidence base for this activity
Chuang E, Pourat N, Haley LA, O’Masta B, Albertson E, Lu C. Integrating Health And Human Services In California’s Whole Person Care Medicaid 1115 Waiver Demonstration. Health Affairs. 2020 Apr 1;39(4):639–48.
Tomoaia-Cotisel A, Farrell TW, Solberg LI, Berry CA, Calman NS, Cronholm PF, et al. Implementation of Care Management: An Analysis of Recent AHRQ Research. Medical Care Research and Review. 2016 Oct 23;75(1):46–65.
Endnotes
- Garite TJ, Manuck TA. Should case management be considered a component of obstetrical interventions for pregnancies at risk of preterm birth? American Journal of Obstetrics and Gynecology [Internet]. 2023 Apr 1 [cited 2024 Jan 16];228(4):430–7. Available from: https://pubmed.ncbi.nlm.nih.gov/36130634/
- https://www.dhcs.ca.gov/CalAIM/ECM/Pages/Home.aspx
- https://www.dhcs.ca.gov/CalAIM/Documents/CalAIM-ECM-a11y.pdf